
Contact Us
-
Establishing Good Oral Care Habits at Every Age
posted: Apr. 27, 2024.

-
Fluoride Treatments—They’re Not Just for Kids!
posted: Apr. 23, 2024.

-
Make Every Day Earth Day
posted: Apr. 16, 2024.

-
Antibiotic Prophylaxis or Premedication
posted: Apr. 09, 2024.

-
Snowball Effect
posted: Apr. 02, 2024.

-
The Top 5 Most Common Dental Issues and Why Early Treatment Matters
posted: Mar. 29, 2024.

-
The Best Brush of the Day
posted: Mar. 26, 2024.

-
I have halitosis. What can I do?
posted: Mar. 19, 2024.

-
St. Patrick's Day
posted: Mar. 12, 2024.

-
Good Nutrition Leads to Healthy Mouths
posted: Mar. 05, 2024.

-
Healthy Gums and Older Adults
posted: Feb. 27, 2024.

-
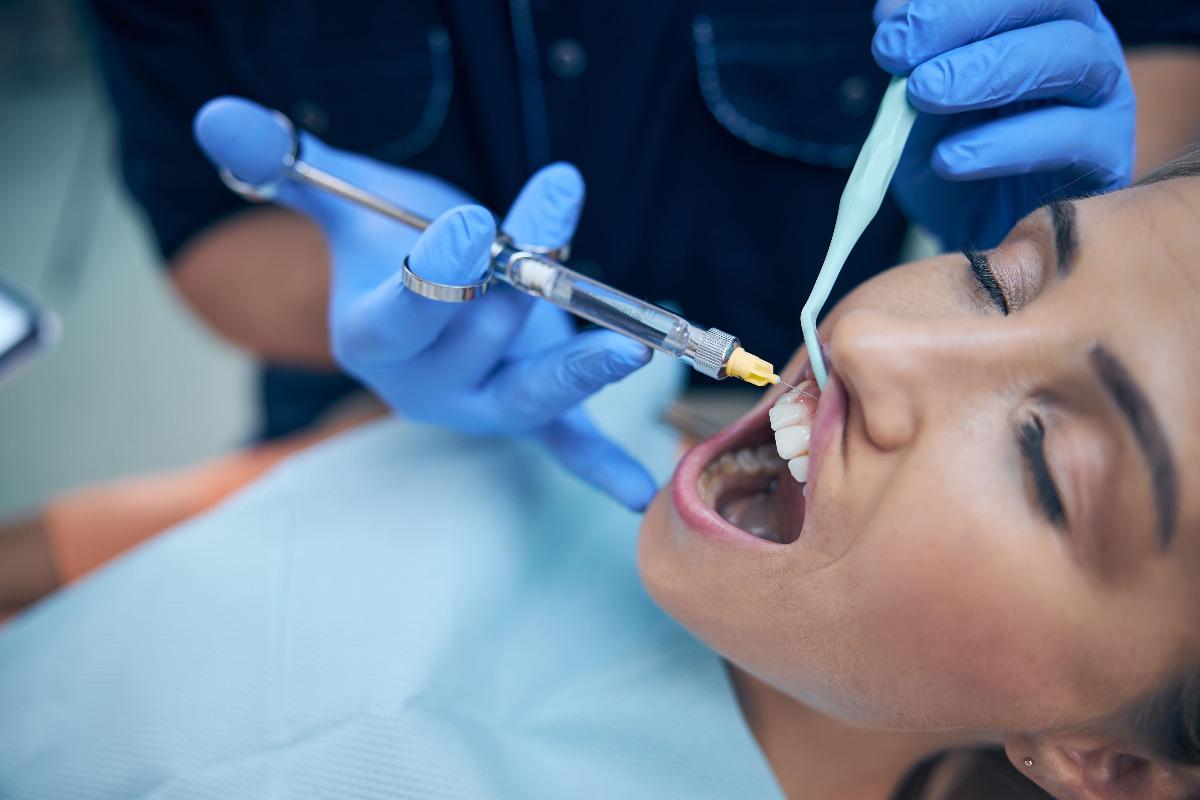
Easing Dental Anxiety: A Look into Dental Anesthesia and Sedation Options
posted: Feb. 24, 2024.
-
The Latest News In Dental Care: A Look into the Future
posted: Feb. 15, 2024.

-
The Origins of Valentine's Day
posted: Feb. 13, 2024.

-
Getting to the Bottom of Chewing Gum Myths
posted: Feb. 06, 2024.

-
Take Your Pick!
posted: Jan. 30, 2024.

Contact Us
Send Us an Email
Our Location
Find us on the map
Hours of Operation
Our Regular Schedule
Monday:
8:00 am-5:00 pm
Tuesday:
8:00 am-5:00 pm
Wednesday:
7:00 am-2:00 pm
Thursday:
7:00 am-2:00 pm
Friday:
Closed
Saturday:
Closed
Sunday:
Closed

